If you have abnormal menstrual bleeding, you may require testing in order to determine the underlying problem.
If you are experiencing abnormal menstrual bleeding, your doctor will likely recommend that you undergo some testing. Blood and urine samples may be collected, and there are a number of ways that the inside of your pelvic organs can be visualized. Knowing what the test will involve can help ease any worries you may have.
What tests are used to help diagnose abnormal menstrual bleeding?
 This list of tests does not include blood tests that you might take, and is specifically referring to physical exam, imaging, radiology, and biopsies. If you have a known bleeding disorder, it is important to tell your doctor so that you may take the proper preparations to ensure that bleeding resulting from a test will be well controlled – particularly in the case of biopsy.
This list of tests does not include blood tests that you might take, and is specifically referring to physical exam, imaging, radiology, and biopsies. If you have a known bleeding disorder, it is important to tell your doctor so that you may take the proper preparations to ensure that bleeding resulting from a test will be well controlled – particularly in the case of biopsy.
Pelvic exam
A pelvic exam allows your doctor to examine your pelvic organs. The position and size of your uterus, ovaries and cervix can also be assessed. After visually inspecting your vulva, vagina, and cervix, your doctor will insert one or two gloved fingers inside your vagina, while using the other hand to press on your lower belly. The doctor will be able to find and feel your uterus and your ovaries. Any unusual growths or painful spots can be identified.
Rectal-vaginal exam
A recto-vaginal exam can be used to feel your ovaries and the ligaments of your uterus. The doctor will insert one finger in your rectum and one in your vagina, in order to feel the tissues deep in your pelvis. This allows the doctor to feel for abnormalities behind the uterus, and on the lower walls of the vagina.
Pelvic ultrasound
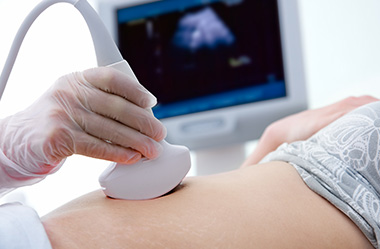
A pelvic ultrasound is used to visualize the organs in the lower pelvis, including the uterus, cervix, fallopian tubes, ovaries, and bladder. The procedure uses sound waves that are emitted from a small, handheld device (transducer) that is placed on your lower abdomen. A gel is applied to your skin to help the sound waves travel better. Sometimes to better visualise the uterus a sterile ultrasound probe is placed in the vagina (transvaginal ultrasound) or rectum (rectal ultrasound). Pelvic ultrasound can help in the diagnosis of abnormal menstrual bleeding, and can be used to view the lining of the uterus. There is no radiation involved in ultrasound.
Transvaginal ultrasound
Transvaginal ultrasound uses sound waves to provide images of the female reproductive organs, including the uterus, cervix, ovaries, fallopian tubes, and pelvic area. A lubricated probe (transducer) will be placed about 5 cm into your vagina. The technician will maneuver the probe in order to capture images of the pelvic organs.
Hysteroscopy
This procedure allows your doctor to see inside your uterus, using an instrument called a hysteroscope. The hysteroscope is a thin tube with a camera and a light on the end, which is inserted in your vagina, through your cervix, and into your uterus. The image is transmitted to a screen and allows your doctor to view the lining of your uterus, and to take a biopsy or remove small polyps. This is usually done in a procedure or operating room, although some new and very small hysteroscopes may allow visualization to be done in office settings.
Hysterosalpingogram
This is a test that involves introducing a special type of dye into your uterus and fallopian tubes, and then taking an x-ray. The dye is inserted through a small tube that the doctor inserts in your vagina, through your cervix, and into your uterus. This test can show whether there are structural abnormalities (e.g., fibroids, polyps) within the uterus. It is also used to see whether your fallopian tubes are open or blocked.
Sonohysterography
This procedure is also called saline infusion sonography. It is very similar to transvaginal ultrasound, except that a doctor will introduce a small amount of sterile saline solution into your uterus prior to the ultrasound procedure. This permits improved viewing of the lining of the uterus.
MRI
An MRI is short for ‘magnetic resonance imaging’, which uses a powerful magnetic field to produce highly detailed images of the body’s internal structures. MRI can be used to help diagnose many of the structural causes of heavy menstrual bleeding, such as fibroids, polyps, endometriosis, and adenomyosis.
Pap smear
This test involves taking a sample of cervical cells and examining them for potentially cancerous cells. Your doctor will open your vagina with a device called a speculum, and use a small plastic spatula and a small brush to collect a sample of cells from your cervix. You may experience cramping during this procedure.
Endometrial biopsy
This procedure involves removing a small sample of tissue from the lining of the uterus in order to assess the health of the endometrium. To do this, your doctor will use a small suction tube, called a pipette. The procedure takes 10-15 minutes, and may cause some cramping. Some vaginal bleeding may occur after the procedure.
Dilatation and curettage
This procedure involves the removal of tissue from the inside of the uterus. It can be used to diagnose or treat some causes of heavy menstrual bleeding, such as fibroids, polyps, or uterine cancer. This may be done in conjunction with a hysteroscopy, in which the uterine cavity is visualized with a camera.
The procedure takes 10-15 minutes, and is conducted under local, spinal, or general anesthesia. The cervix is opened (dilated) with an instrument or a medication, and a spoon-shaped instrument called a ‘curette’ is inserted into the uterus and used to scrape the uterine lining. Suction may be used to remove the contents. You may experience cramping and bleeding after the procedure. This usually only lasts for a day or two. This is rarely needed to diagnose a bleeding disorder.
Colonoscopy
A colonoscope is a thin, flexible tube, with a camera and a light on the end of it. It is inserted into your rectum and can be used to visualize up to six feet of colon and small intestine. The images are transmitted to a screen, so your doctor can see the inside of bowel. Your doctor will be able to see if endometrial tissue is present within your colon. This is rarely needed to diagnose a bleeding disorder.
Cystoscopy
A cystoscope is a thin tube, with a camera and a light on the end. It is inserted into your urethra, up into your bladder, and is used to transmit images of the inside of your bladder to a screen for your doctor to see. Your doctor will be able to see if there is endometrial tissue inside your bladder. This is rarely needed to diagnose a bleeding disorder.

